Medically reviewed by
What is testicular cancer?
Testicular cancer is caused by the abnormal development of cells in the testes (also known as testicles), which results in the formation of so-called testicular germ cell tumours (TGCTs).
Testicular cancer occurs in 1 in 25,000-30,000 Australian men. Around 900 Australian men are diagnosed with testicular cancer each year and almost 90% of them are aged under 50 years.
Although testicular cancer accounts for less than 1% of cancers in men, it’s the most common type of tumour in men aged in their 20s and 30s.
Symptoms of testicular cancer
The most common symptom of testicular cancer is a lump that can be felt on, or enlargement or hardening of, one testicle (testicular cancer usually doesn’t occur on both sides). The lump may or may not be painful.
Some men with testicular cancer that has metastasised might not seek help until they have severe symptoms, like weight loss, breathlessness or coughing blood.
Scrotum and testicular anatomy
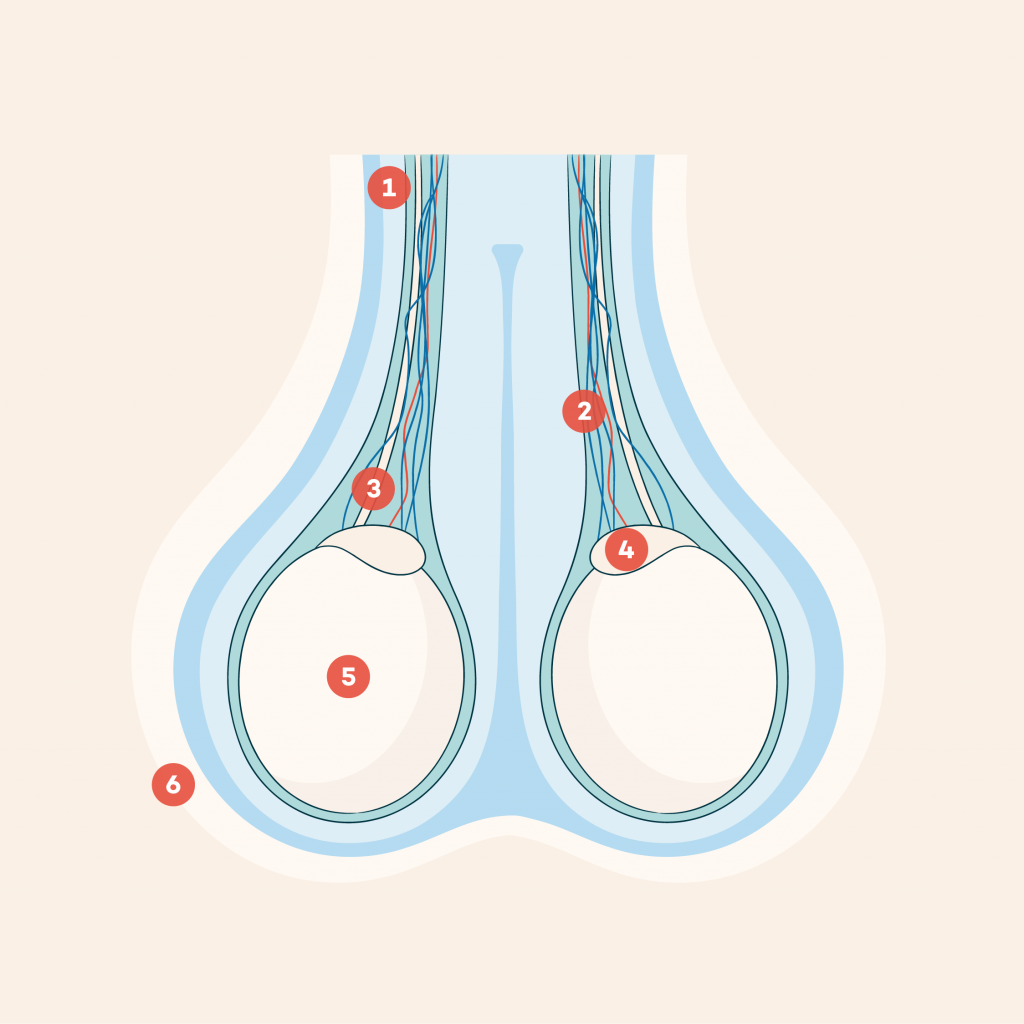
Anatomy key
- Spermatic tube
- Testicular arteries and veins
- Vas deferens
- Epididymis
- Testis
- Scrotum
Causes of testicular cancer
Many characteristics of testicular cancer suggest that the disease begins in early life, from genetic changes in the stem cells that usually go on to form sperm.
Testicular cancer is more common in boys and men with abnormalities in genital development, including cryptorchidism and hypospadias, than in those without.
Diagnosis of testicular cancer
Testicular cancer is diagnosed through an ultrasound to examine a testicular lump, and blood tests to measure molecules that indicate the presence of cancer.
MRI or CT scans are used to look for the spread of cancer to other parts of the body.
Subscribe to our newsletter

Treatment of testicular cancer
If you have testicular cancer, you’ll usually have surgery to remove the affected testicles (orchidectomy). This cures most men with tumours that have not spread outside of the testicle. You can have a prosthetic testicle inserted so the appearance of your genitals is not affected.
If your testicular cancer has spread to nearby lymph nodes or other parts of the body, your treatment will usually include radiotherapy or chemotherapy as well as surgery to remove the tumour. Biopsy of tissues might be needed to confirm if the cancer has spread.
Health effects of testicular cancer
Almost all men with testicular cancer that hasn’t spread are cured by orchidectomy, although some need chemotherapy or radiotherapy as well, depending on the tumour type.
Most men with testicular cancer that has metastasised are cured by chemotherapy, but 20-30% may relapse and need further treatment.
97% of all men diagnosed with testicular cancer survive for at least another five years.
Chemotherapy and radiotherapy can affect your fertility, so you might need to think about taking steps to preserve your fertility, such as sperm banking, before your treatment begins.
What to do about testicular cancer
You should regularly perform a testicular self-examination (TSE). A TSE is a quick and simple process.
You might find it easier after a warm bath or shower, when the skin of your scrotum is relaxed.
Stand in front of a mirror. To start with, check for any swelling on the skin of your scrotum. Hold your scrotum in your hands and feel the size and weight of each testicle.
Don’t worry if one testicle is a little bigger or hangs lower than the other, that’s normal.
Feel each ball and roll it between your thumb and finger, one at a time, checking for any lumps or swelling.
The testicles should feel firm, and the surface should feel smooth. You should be able to feel your epididymis, a soft tube toward the back of each testicle that carries sperm to the ejaculatory ducts.
Check for any swelling in this area. You shouldn’t feel any pain when checking your testicles.
See your doctor if you notice any changes, pain or discomfort.