Our personal experiences tell us that the COVID-19 pandemic and its management affected our well-being, and this is backed up by analysis of available evidence. Although the data are not ideal, rates of anxiety, depression, psychological distress, and post-traumatic stress disorder are consistently higher than normal, with females, children and adolescents, and disadvantaged groups most affected1,2,3.
It’s easy to see how concerns about increasing rates of suicide stem from this situation.
Early in the pandemic, mental health experts warned of an impending increase in suicides — on top of our already tragically high rates — and called for better collection and reporting of suicide statistics to help respond4,5. There’s a lag of up to 18 months in the reporting of suicides in Australia6 but a National Suicide and Self-harm Monitoring System is being established to reduce that lag7.
Suicide registers from Victoria, New South Wales and Queensland do not show a rise in suicide rates during the first months of the COVID-19 pandemic9 although police reports from Queensland suggest the situation was a contributory factor in some suicides since the beginning of the outbreak10.
The data from Australia are consistent with those from a variety of sources from around the world. A recent analysis of ‘real-time’ suicide data from 21 countries shows no increase in suicides during the early months of the pandemic for any of the countries or regions examined11. In fact, suicide rates were lower than expected in 12 countries or regions, including NSW.
Accurate and timely reporting of data has been critical for managing the global COVID-19 pandemic. The public has come to expect, and appreciate, accuracy and detail in reporting of health data. Of course, the positive news about suicide rates during the COVID-19 pandemic should not make us complacent.
Perhaps the anticipated increase in suicides was averted by investments in mental health services in the early stages of the pandemic. Maybe the collective community response to the pandemic provided support or reassurance to people at risk.
Hopefully, the predicted rise in suicides isn’t just delayed.
Data from the suicide registers in Victoria, NSW, and Queensland remind us about the deficiencies in reporting health data. Victoria is the only jurisdiction to provide up-to-date information broken down by gender.
Examination of the data (see figure 1) shows an apparent decrease in suicide by women over the most recent 12-month period to 30 September 2021 but no change for males. In males aged over 65 years, suicides seem to have increased from an average of 50 per year before 2020, to just over 70 per year since.
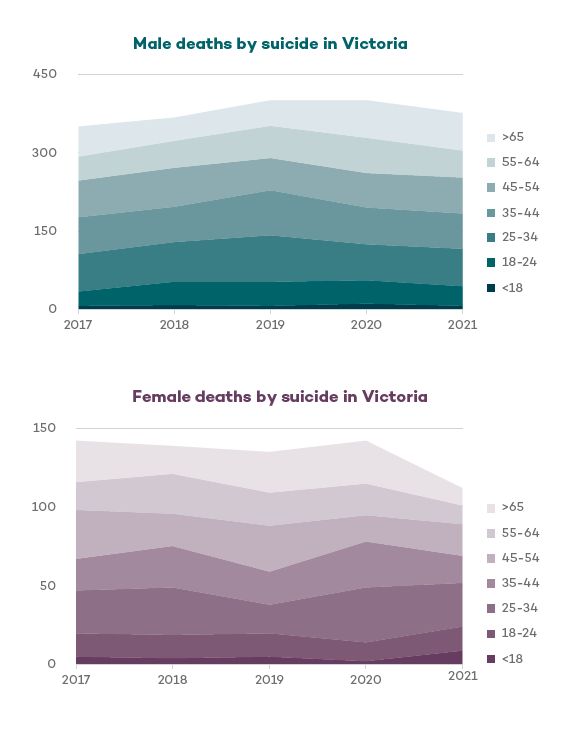
A failure to break down statistics by gender, for any health condition or outcome, can hide important information and prevent necessary responses. Information about such a profound influence on health and the effects of disease is critical for interventions to be sufficiently tailored to properly address gender disparities in health and wellbeing.
Read more: What COVID-19 really means for men’s health
References
[1] Salari et al., 2020. Prevalence of stress, anxiety, depression among the general population during the COVID-19 pandemic: a systematic review and meta-analysis. Globalization and Health
[2] Rodríguez-Fernández et al., 2021. Psychological Effects of Home Confinement and Social Distancing Derived from COVID-19 in the General Population—A Systematic Review. International Journal of Environmental Research and Public Health
[3] Xiong et al., 2020. Impact of COVID-19 pandemic on mental health in the general population: A systematic review. Journal of Affective Disorders
[4] https://www.abc.net.au/news/2020-05-07/national-suicide-register-needed-coronavirus-surge/12208668
[5] John et al., 2020. Trends in suicide during the covid-19 pandemic. BMJ
[6] https://www.aihw.gov.au/suicide-self-harm-monitoring/data/suicide-self-harm-monitoring-data
[10] Leske et al., 2021. Real-time suicide mortality data from police reports in Queensland, Australia, during the COVID-19 pandemic: an interrupted time-series analysis. The Lancet Psychiatry
[11] Pirkis et al., 2021. Suicide trends in the early months of the COVID-19 pandemic: an interrupted time-series analysis of preliminary data from 21 countries. The Lancet Psychiatry










